Choosing the right approach to customer experience in healthcare is rarely straightforward. For Chief Customer Officers across North American healthcare organizations, the stakes go far beyond service—they touch every aspect of patient trust, clinical outcomes, and long-term loyalty. Customer experience shapes patient engagement at every touchpoint, blending clinical quality with service excellence in ways that can set your organization apart. Knowing how to define and measure this journey is essential in meeting today’s rising patient expectations and driving meaningful results.
Table of Contents
- Defining Customer Experience In Healthcare CX
- Major Variations And Patient Engagement Models
- Key Benefits For Patient Outcomes And Loyalty
- Practical Risks And Impact On Retention
- Common Mistakes In Healthcare Experience Design
Key Takeaways
| Point | Details |
|---|---|
| Comprehensive Customer Experience | Customer experience in healthcare includes every interaction across all touchpoints, significantly influencing patient trust and treatment adherence. |
| Engagement Models Matter | Different patient populations require tailored engagement models that prioritize collaboration and co-creation with providers. |
| Impact on Patient Loyalty | Seamless patient experiences lead to improved loyalty, adherence to treatment, and overall clinical outcomes, highlighting the need for strategic experience design. |
| Risks of Poor Experience | Poor patient experiences result in financial losses and decreased retention, emphasizing the importance of addressing experience gaps proactively. |
Defining Customer Experience in Healthcare CX
Customer experience in healthcare isn’t a single moment or transaction. It’s the complete journey patients navigate from their first awareness of a provider through ongoing care and beyond.
Customer experience encompasses every interaction—clinical and non-clinical—across all touchpoints. This includes scheduling appointments, waiting room experiences, clinician communication, billing interactions, and post-care follow-ups.
Unlike retail or other industries, healthcare customer experience carries higher stakes. Patients are often vulnerable, stressed, or managing chronic conditions when they engage with your organization. Their experience directly influences whether they trust your clinical recommendations, comply with treatment plans, and return for future care.
Research shows that customer experience in healthcare extends beyond simple satisfaction metrics. It involves how patients perceive service quality, how they co-create value with providers, and whether they feel heard throughout their healthcare journey.
For Chief Customer Officers leading North American healthcare organizations, this distinction matters significantly:
- Patient engagement increases when experience aligns with expectations at every touchpoint
- Clinical outcomes improve when patients feel respected and understood by care teams
- Loyalty strengthens when organizations consistently deliver on both clinical and service promises
- Operational efficiency gains emerge when friction points are eliminated from patient pathways
The modern patient arrives with different expectations than previous generations. They research providers online, compare experiences on social platforms, and expect omnichannel communication options. They want transparent pricing, streamlined administrative processes, and providers who acknowledge their time constraints.
Patient experience shapes whether they become advocates for your organization or seek care elsewhere. In healthcare, this directly impacts revenue, reputation, and patient outcomes.
Defining customer experience for your organization means clearly articulating what you promise patients at each interaction stage. It requires understanding your current state through patient feedback, identifying gaps between expectations and reality, and prioritizing improvements that matter most to your patient population.
When customer care teams understand this definition deeply, they become extensions of your clinical mission. They’re empowered to solve problems, prevent escalations, and create moments patients remember positively.
Pro tip: _Start by mapping your patient journey from initial contact through post-care follow-up. At each stage, identify what matters most to patients and where friction currently exists. This creates your baseline for measuring customer experience improvements.
Major Variations and Patient Engagement Models
Patient engagement isn’t one-size-fits-all. Healthcare organizations operate across different contexts, patient populations, and care settings, each requiring distinct engagement approaches.

Patient engagement models vary widely in structure and scope, but they consistently emphasize collaboration between patients and providers. These frameworks span from individual patient-provider relationships to organization-wide systems and broader policy contexts.
What separates effective engagement from ineffective efforts is understanding where your organization operates within these models. A primary care clinic’s engagement strategy differs fundamentally from a hospital system managing complex, multi-specialty patients or a behavioral health organization working with vulnerable populations.
Key variations you’ll encounter include:
- Intrapersonal engagement focuses on individual patient motivation and health literacy
- Interpersonal engagement strengthens direct relationships between patients and clinical teams
- Organizational engagement integrates patient input into service design and operational decisions
- Systemic engagement shapes policy and healthcare delivery across multiple institutions
Patient co-creation represents another critical dimension. This moves beyond passive feedback to active patient involvement in designing care pathways, treatment options, and service delivery methods.
Many organizations struggle here. They collect patient surveys but don’t act on insights. They create advisory boards but don’t empower them to drive change. True co-creation requires genuine shared decision-making where patient values directly influence clinical protocols and operational choices.
Different patient populations require different engagement models. What resonates with geriatric patients managing chronic conditions differs dramatically from engaging younger patients with acute care needs.
Your patient demographic shapes which model works best. Age, health literacy, cultural background, and condition complexity all influence how patients want to engage. A patient with diabetes needs different engagement touchpoints than one undergoing surgical recovery.
When customer service best practices align with your chosen engagement model, teams deliver consistent experiences. They know which patients need more frequent communication, which prefer autonomy, and which require additional support navigating complex decisions.
Implementing multiple models simultaneously creates organizational flexibility. You’re not forcing one engagement approach on all patients. Instead, you’re offering pathways that match individual preferences and clinical needs.
Here’s a comparison of patient engagement models and their typical applications:
| Engagement Model | Core Focus | Example Setting | Typical Patient Need |
|---|---|---|---|
| Intrapersonal | Individual motivation | Outpatient clinics | Health literacy boost |
| Interpersonal | Patient-clinician relationship | Specialty practices | Clear communication |
| Organizational | Patient input in operations | Hospital systems | Service design participation |
| Systemic | Policy and delivery integration | Health policy networks | Access and equity priorities |
Pro tip: _Audit your current patient population by engagement type. Identify which models dominate your existing patient base, then assess whether your customer service teams are equipped to support those specific engagement approaches effectively.
Key Benefits for Patient Outcomes and Loyalty
When patients experience seamless, respectful interactions throughout their healthcare journey, something measurable shifts. They become more invested in their own care, more likely to follow treatment recommendations, and significantly more loyal to your organization.

The connection between customer experience and clinical outcomes isn’t theoretical. Patient loyalty improves through satisfaction and service quality, creating a direct pathway to better health results. Loyal patients commit to ongoing relationships with providers and adhere more consistently to treatment plans.
Consider the practical impact. A patient who trusts your organization follows medication schedules more reliably. They attend scheduled appointments instead of missing them. They communicate openly about side effects or concerns rather than abandoning treatment silently.
These behaviors compound into measurable clinical improvements:
- Treatment adherence increases when patients feel heard and respected during consultations
- Health outcomes improve as patients commit to care plans they helped design
- Preventive care utilization rises when patients understand value and feel supported
- Hospital readmission rates decline when discharge communication and follow-up are coordinated thoughtfully
- Medication errors decrease through transparent communication about medications and side effects
Your customer experience strategy directly influences these metrics. When appointment scheduling feels frictionless, patients show up on time. When billing is transparent, patients don’t avoid follow-up care due to cost anxiety. When clinical teams listen to patient concerns, patients disclose important health information.
Patient engagement fosters open communication and collaborative care, which drives treatment adherence and satisfaction simultaneously. This isn’t separate from clinical work—it amplifies it.
Loyal patients aren’t just revenue generators. They’re your organization’s most effective advocates, referring family and friends while maintaining longer-term relationships.
Loyalty also reduces operational friction. Repeat patients require shorter intake processes. They maintain updated information in your systems. They’re more forgiving of occasional service gaps because they’ve experienced your overall value.
For Chief Customer Officers, this means framing customer experience as a clinical strategy, not a soft service improvement. Revenue grows because outcomes improve and patients return, but the primary driver is better health.
Pro tip: _Track patient outcome metrics alongside experience scores. Measure treatment adherence rates, preventive care completion, and hospital readmission data correlated with patient satisfaction. This evidence builds clinical leadership buy-in for continued investment.
Practical Risks and Impact on Retention
Poor patient experience doesn’t just damage relationships—it actively drives patients away. The financial and clinical consequences ripple through your entire organization, affecting revenue, staff morale, and clinical outcomes.
Patients leave when they encounter friction at critical moments. A missed follow-up appointment reminder means they forget their visit. A confusing billing statement makes them question whether your organization values transparency. A rushed consultation leaves them feeling unheard, questioning whether they should seek care elsewhere.
Communication breakdowns and coordination failures create patient frustration that undermines trust and continuity of care. These operational gaps directly trigger patient churn and reduce retention rates across your system.
Specific retention risks include:
- Missed appointments stemming from unclear communication about scheduling or location changes
- Billing confusion when patients receive unexpected charges or don’t understand insurance coverage
- Long wait times that signal your organization doesn’t respect patient schedules
- Communication silence during treatment gaps or between visits, leaving patients feeling abandoned
- Rushed clinical interactions where patients sense they’re being processed rather than cared for
Each instance erodes trust. Repeat them, and patients switch providers. North American healthcare markets are increasingly competitive—patients have options and aren’t reluctant to exercise them.
The financial impact is substantial. Acquiring new patients costs significantly more than retaining existing ones. When a patient leaves, you lose not just their current revenue but future visits, referrals, and lifetime value. A patient with chronic conditions who switches providers represents hundreds of thousands in lost long-term revenue.
Beyond finances, patient churn results from unclear communication and rushed experiences that diminish emotional connection and trust. Reducing churn depends on consistently making patients feel respected and supported throughout their healthcare journey.
Every patient who leaves your organization takes feedback with them. They share their negative experience with an average of nine other people, influencing their healthcare decisions.
Staff burnout intensifies when patient dissatisfaction rises. Teams handling angry calls about billing issues or confused patients get demoralized. High turnover in customer-facing roles then creates even worse experiences, accelerating churn further.
Prevention is far simpler than recovery. Addressing experience gaps before patients leave costs a fraction of replacing them.
The following table summarizes common risks in poor healthcare experience and their downstream consequences:
| Risk Factor | Immediate Effect | Long-Term Impact |
|---|---|---|
| Missed appointments | Care gaps | Higher readmission rates |
| Billing confusion | Patient frustration | Reduced retention |
| Long wait times | Lost trust | Negative word-of-mouth |
| Rushed interactions | Feeling unheard | Lower treatment adherence |
Pro tip: _Monitor your patient churn rate by department and interaction type. Identify which touchpoints show highest abandonment, then prioritize improvements there first. Quick wins build momentum while larger system changes develop.
Common Mistakes in Healthcare Experience Design
Many healthcare organizations approach experience design with good intentions but flawed execution. They optimize one piece without considering how it connects to the whole patient journey, creating disconnects that frustrate patients and staff alike.
The most damaging mistake is overlooking clinicians. Organizations design patient journeys without consulting the teams delivering care. This creates workflows that look good on paper but create operational chaos for frontline staff, ultimately harming patient experience when stressed clinicians rush through interactions.
Overlooking clinician roles and multi-dimensional context results in experience designs that fail in real-world settings. Effective design requires integrating perspectives from patients, clinicians, administrative staff, and support teams across intrapersonal, interpersonal, organizational, and policy levels.
Common design pitfalls include:
- Siloed improvement efforts where departments optimize independently without coordinating handoffs
- Ignoring emotional and environmental context by focusing only on transactional efficiency
- Designing interfaces patients don’t understand, leading to confusion and errors
- Unclear workflows that create decision points where patients feel lost or anxious
- Inaccessible tools that exclude patients with limited technology skills or disabilities
Poorly designed patient portals exemplify this mistake. Organizations launch slick interfaces patients can’t navigate. Appointment scheduling requires five clicks when it should take two. Billing statements use jargon instead of plain language. Then organizations blame patients for not using the tools instead of recognizing design failures.
Design errors occur when patient empowerment is neglected, leaving patients confused and lacking control. Designing for empowerment requires clear communication, intuitive workflows, and tools that give patients confidence navigating healthcare interactions independently.
The best healthcare experience design feels invisible. Patients accomplish what they need without wondering whether they’re using the system correctly.
Another critical mistake is treating experience design as a marketing project rather than an operational transformation. You can’t layer nice communication on top of broken systems. If appointment scheduling is fragmented across multiple platforms, no friendly email will fix patient frustration.
Many organizations also neglect measuring what matters. They track satisfaction scores without correlating them to actual behavior changes like appointment adherence or patient retention. This creates the false impression that small improvements are sufficient when systemic issues remain.
Pro tip: _Before designing new experiences, map current workflows through the eyes of both patients and clinicians. Identify where their needs conflict, then resolve those conflicts first. This prevents designing solutions that work theoretically but fail operationally.
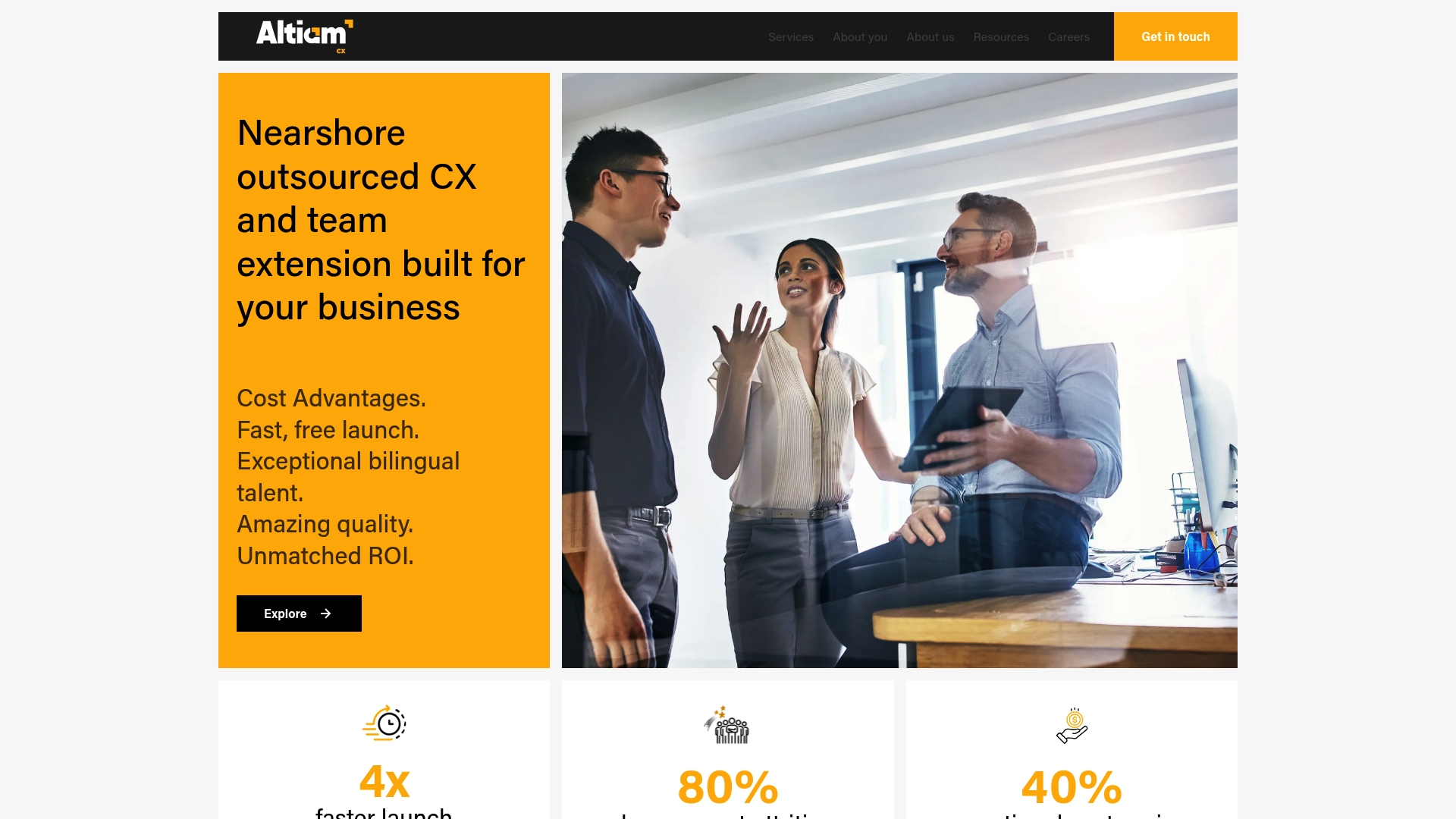
Elevate Your Healthcare Customer Experience with Altiam CX
The article highlights a critical challenge healthcare organizations face today: delivering seamless and compassionate customer experiences that drive patient loyalty, improve clinical outcomes, and reduce costly churn. Key pain points include communication breakdowns, complex patient engagement models, and operational inefficiencies that cause frustration and disengagement. Terms like “patient co-creation,” “customer care teams,” and “patient journey mapping” emphasize the depth of transformation needed to truly align with patient expectations and clinical goals.
Altiam CX understands these challenges deeply. As your strategic nearshore partner, we provide customer care, technical assistance, and back-office operations designed specifically to reduce friction and enhance service quality across every touchpoint. Our culturally aligned and disciplined approach empowers your teams to deliver personalized experiences that patients trust and value. By integrating performance frameworks that measure outcomes alongside experience, we help healthcare organizations transform patient journeys into thriving pathways of engagement and loyalty.
Ready to turn the insights from “Why Customer Experience Matters in Healthcare CX” into action? Explore how Altiam CX can help your healthcare organization streamline workflows, elevate patient communication, and foster lasting loyalty.
Partner with Altiam CX today to empower your customer care teams and unlock the full potential of your patient relationships. Visit Altiam CX now to start your journey toward better healthcare experiences.
Frequently Asked Questions
What is customer experience in healthcare?
Customer experience in healthcare refers to the entire journey a patient goes through, including all interactions with the healthcare provider, from initial awareness to ongoing care.
Why is customer experience important in healthcare?
Customer experience is vital in healthcare because it influences patient trust, compliance with treatment plans, loyalty to the provider, and ultimately, clinical outcomes.
How can healthcare organizations improve patient engagement?
Healthcare organizations can improve patient engagement by tailoring their approach to different patient populations, involving patients in decision-making, and ensuring effective communication across all touchpoints.
What are the consequences of poor patient experience?
Poor patient experience can lead to missed appointments, decreased patient loyalty, higher churn rates, and negative impacts on clinical outcomes, which can ultimately affect an organization’s revenue and reputation.
Recommended
- 7 Customer Service Best Practices for Healthcare CX Leaders
- Healthcare Customer Experience Outsourcing: What Providers Expect in 2026
- Role of Customer Care Teams: Enhancing Healthcare and Ecommerce
- CX & Operational Support for Health Systems
- The United Healthcare Cyber Breach: A Wake-Up Call for Cybersecurity in the Insurance Industry